Breakthrough pill for Parkinson’s could treat disease early and relieve symptoms without side-effects
- It is a combination of two Parkinson’s drugs – pramipexole and rasagiline
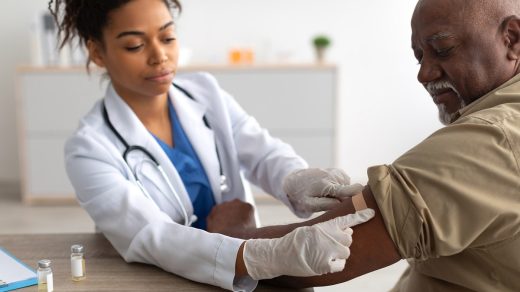
A daily capsule could treat Parkinson’s disease early and relieve symptoms — without the side-effects of standard drug treatments.
It involves a combination of two existing Parkinson’s medications, pramipexole and rasagiline, given at low doses in a slow-release formula.
The idea is that their complementary mechanisms work together to increase levels of dopamine in the brain — a key trigger of the disease.
The fact that low doses are used means the drugs won’t cause the unpleasant side-effects they do when used alone at much higher doses. These can include muscle spasms or weakness, nausea, dizziness and sleep problems.
In a recent trial, patients who took the new low-dose combination medication, known as P2B001, experienced the same improvements in their symptoms as seen with a standard treatment, but had significantly fewer side-effects.

A daily capsule could treat Parkinson’s disease early and relieve symptoms — without the side-effects of standard drug treatments (file photo)
And if P2B001 is approved by the regulatory authorities, it could mean patients receive drug therapy as soon as they are diagnosed, rather than being monitored until symptoms worsen.
Currently, many doctors wait until symptoms are more severe before starting drug therapy in order to avoid patients developing complications such as dyskinesia (e.g. jerks and tremors).
A 2009 study in the journal Archives of Neurology found that 50 per cent of those on pramipexole alone developed dyskinesia.
Parkinson’s disease is caused by a loss of nerve cells in the brain that produce dopamine, a chemical messenger that helps control body movement.
If these cells become damaged or die, levels of dopamine are reduced and movements become slow and abnormal, leading to tremors and balance problems that worsen over time.
Drugs used to treat Parkinson’s, such as levodopa, work by increasing dopamine levels. While these can keep symptoms at bay for years, they can also have side-effects.
P2B001 is a combination of pramipexole and rasagiline in low doses, which are released slowly to maintain a constantly high level of dopamine throughout the day.
The two were chosen for their complementary mechanisms: while pramipexole works by mimicking the effects of dopamine, rasagiline effectively blocks the enzymes responsible for breaking down dopamine.
In a study with newly-diagnosed Parkinson’s patients, 147 received P2B001 and 72 were treated with pramipexole alone.
After 12 weeks, there was a similar improvement in symptoms in both groups, but the P2B001 group reported significantly fewer side-effects such as nausea, dizziness and heart rhythm problems — and, most notably, less daytime sleepiness.
‘The sum of the parts is much greater than the individual components themselves,’ said Lawrence Elmer, a professor of neurology at the University of Toledo in the U.S., who presented the trial’s results at a recent conference of the American Academy of Neurology.
‘One of the biggest questions for clinicians who treat Parkinson’s patients is, “What do I start newly diagnosed patients on, and when do I start them?”,’ he said.
‘This inability of clinicians to know what to start patients on leads to an increase in the cost of caring for these patients because they are inadequately managed.’
He added: ‘The goal was to design a compound that literally could be given to every newly diagnosed patient with Parkinson’s, that will work in the vast majority of those patients, with the best tolerability I’ve seen in a compound in almost 20 years.’
Claire Bale, of the charity Parkinson’s UK, told Good Health: ‘The results from the recent trial show that giving the two drugs together provides better symptom control than using either alone and seems to have fewer side effects.’
She added that a big advantage of P2B001 is that it’s taken just once a day.

Currently, many doctors wait until symptoms are more severe before starting drug therapy in order to avoid patients developing complications such as dyskinesia (e.g. jerks and tremors)
‘Many people with Parkinson’s take multiple medication throughout the day,’ she explained, ‘so if this new drug could reduce this burden, then that would be a significant step forward.’
The manufacturer, Pharma Two B, plans to submit for approval to market the drug in the U.S. soon; Claire Bale predicts it could take one to two years for the drug to be available in the UK.
Another promising line of research is repurposing medicines — that is, testing drugs originally designed to treat other conditions for their potential use in Parkinson’s.
Large clinical trials under way include testing cholinesterase inhibitors (used to treat memory problems in Alzheimer’s) to see if they can help improve walking and prevent falls in those diagnosed with Parkinson’s.
There are ongoing studies, too, into the diabetes drug exenatide and the cough medication ambroxol as possible treatments for slowing the progression of Parkinson’s.
Another option involves transplanting new dopamine-producing cells, grown from human stem cells in a laboratory.
A ground-breaking study in animals, led by Roger Barker, a professor of clinical neuroscience at Cambridge University, showed this approach to be safe and effective at reversing motor deficits.
Professor Barker told Good Health: ‘In the future, people with Parkinson’s could have a stem cell derived dopamine transplant.
‘You then won’t need to take any drugs because the dopamine cells will be doing the job the drugs are currently doing.
‘Stem cell-derived dopamine cells are designed to repair and replace the lost dopamine cells. They will keep the disease at bay and, for a lot of older patients, this will be a virtual cure.’
This news item came from: https://www.dailymail.co.uk/health/article-12307599/Breakthrough-pill-Parkinsons-treat-disease-early-relieve-symptoms-effects.html